Oregon Health Authority reports early success and capacity strain for Medicaid rent and utility benefit
Loading...
Summary
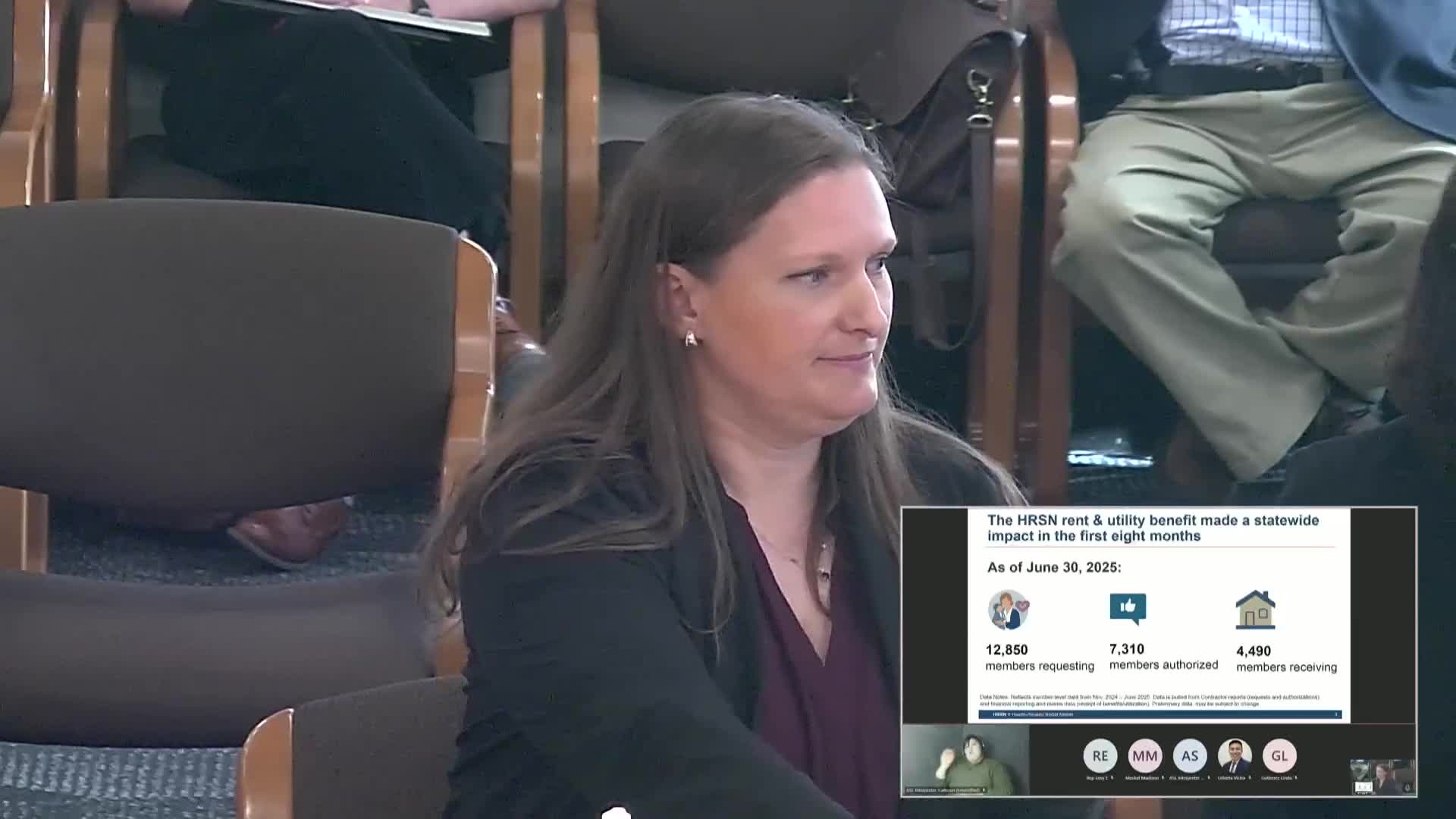
OHA told lawmakers the state's HRSN rent‑and‑utility Medicaid benefit has processed thousands of requests since its Nov. 2024 launch, with over 7,300 approvals and nearly 4,500 members served through June 30, 2025, but implementation faces delays in denser regions due to provider capacity and Medicaid billing workflows.
The Oregon Health Authority briefed the committee on the Health‑Related Social Needs rent and utility benefit launched under the 11‑15 OHP waiver on Nov. 1, 2024.
Amanda Peden, who manages Social Health Needs and Analytics at OHA, said the available member‑level data through June 30, 2025 show more than 12,800 members requested the rent/utility benefit; 7,310 met eligibility and were approved; and nearly 4,500 OHP members had received the benefit in that period. Peden said county rates indicate particularly high relative use in some Northeastern and Southwest coastal counties, and that initial reports from Wheeler County showing zero claims were later updated with preliminary data showing activity there.
OHA and CCO partners acknowledged early operational successes and systemic strain. Jessie Wilson (OHA 11‑15 Waiver Strategic Operations Director) cited capacity constraints and workflow frictions that delay referrals in more densely populated areas, and described a mix of short‑term fixes including community capacity building funds, increased provider reimbursement rates for tenancy supports and onboarding more housing providers. OHA reported providing over $37,000,000 to 161 organizations in 2024 and more than $57,000,000 in 2025 (including $6.3 million in expedited funds for housing providers and $6.9 million to CCOs).
CCO presenters described different local approaches. Josh Balak (AllCare Health) showed a client video and a beneficiary account in which a participant said, "I was able to qualify for that, thank goodness," describing stabilized housing and recovery after receiving six months of rent support. AllCare said it approved over 700 people locally and attributed faster delivery to a smaller, locally integrated model, a landlord payment platform, and concentrated staffing.
Jeremiah Rigsby (CareOregon) described metro‑area scaling challenges: CareOregon reported heavy demand and high call volumes (about 800 calls per day related to HRSN services) and said community partners have limited capacity to accept referrals, requiring ongoing recruitment and operational adjustments.
OHA told lawmakers the waiver authority to provide the HRSN benefit runs through Sept. 2027 and the agency plans to continue operations while monitoring federal guidance and improving workflows. OHA said it will publish more recent data as claims lag resolves and continues onboarding community providers and technical assistance to improve billing and service delivery.
The committee requested additional follow‑up data on provider performance, county‑level service rates and the evolving referrals pipeline; OHA said it will post more data on its website and continue coordination with CCOs and community partners.