HR: State employee medical premiums rose 9%; wellness program and drug trends cited as drivers
Get AI-powered insights, summaries, and transcripts
Subscribe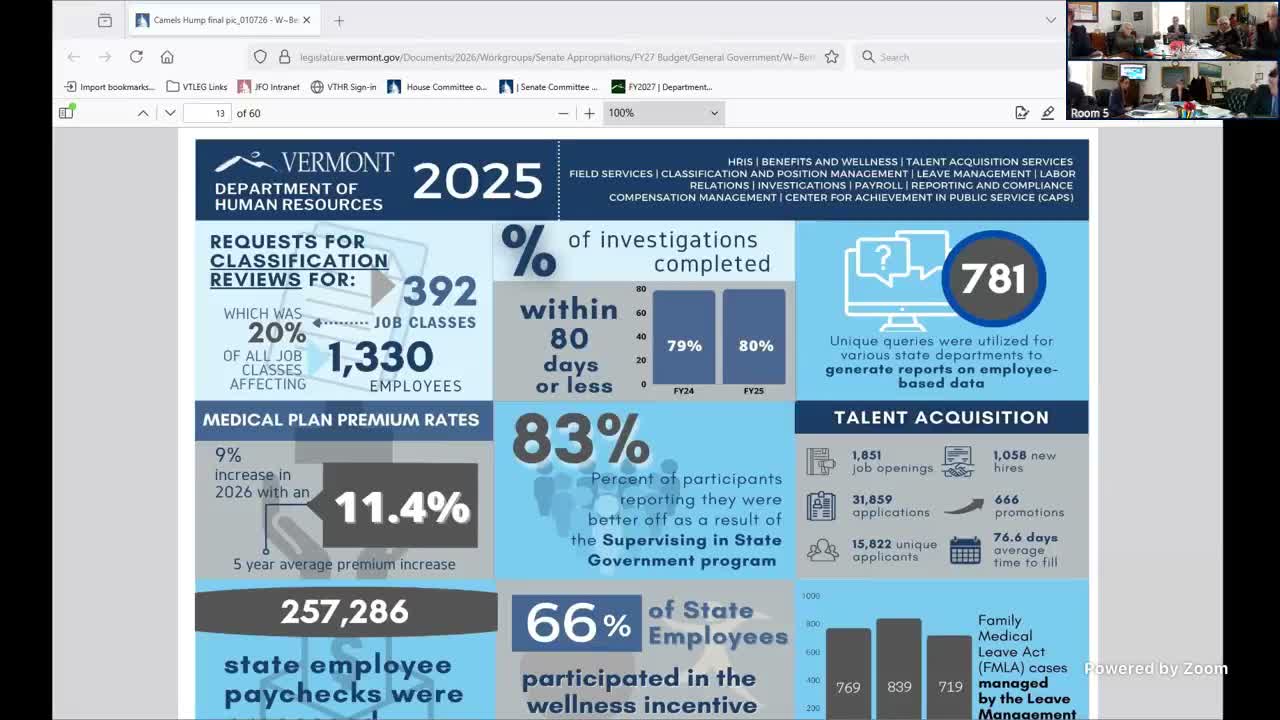
Summary
Commissioner Beth Bastigy told the Appropriations panel that state medical plan premiums rose about 9% for the year and attributed much of the increase to hospital costs and broader use of GLP‑1 weight‑loss drugs; the employer currently pays roughly 80% of premiums.
State Human Resources Commissioner Beth Bastigy told the Senate Appropriations Committee on Jan. 27 that medical plan premium rates increased about 9% for calendar year 2026 and that the rise is a major driver of the department's budget pressures.
Bastigy said, “medical plan premium rates, this year, they increased 9%,” and explained that hospital costs and recent increases in the use of GLP‑1 drugs (previously used to treat diabetes but increasingly prescribed for weight loss) are notable cost drivers. She added that, on average, employees pay roughly 20% of premium costs while the employer covers about 80%, a split that means premium increases are reflected across departmental budgets.
Bastigy described the department's wellness program as a cost‑management and employee‑health tool: the program includes biometric screenings, flu and COVID vaccination clinics, and a points-based incentive system that can yield a modest health‑care credit for employees who participate.
Context and governance: The department said it meets quarterly with labor partners and a benefits advisory committee to review cost drivers and consider plan design changes. Bastigy emphasized the advisory process but did not present a proposed change to plan design during this hearing.
Next steps: HR said it will continue regular benefits monitoring with the benefits advisory committee and labor partners. No committee action on benefits or plan design was recorded in the transcript.
