Local coalitions and treatment programs report early wins from opioid settlement funding; lawmakers weigh sustainability
Loading...
Summary
Representatives of community coalitions, health centers, jails and hospitals described outcomes from opioid‑settlement grants: expanded prevention coalitions, increased access to medication‑assisted treatment across rural health centers, jail MAT programs reaching thousands, and ED‑based MOUD paths. Presenters stressed continued funding is needed to sustain staff and services.
Multiple presenters told the Social Services Appropriations Subcommittee on Jan. 22 that three years of opioid‑settlement funding have seeded prevention coalitions and expanded access to medication‑assisted treatment (MAT) in rural and underserved areas.
Prevention coalitions. Jordan Mathis summarized growth in evidence‑based community coalitions: the state has 23 coalitions with a mix of new and matured groups focused on upstream prevention strategies. Mathis cited a longitudinal example in Panguitch that linked community interventions to declines in self‑reported youth alcohol use over several years.
Community health centers and OUD treatment. Brett Hilton and Rachel Craig said eight community health centers that began receiving funding in late 2023 now serve about 1,500 OUD patients and employ 12 FTEs supported by the grants. They described a roughly 60% increase in new OUD patients at funded centers and said the clinics provide low‑barrier MAT, behavioral health integration, transportation supports and vouchers for uninsured patients. They warned that cuts of 25–60% to settlement funding would reduce visits and could force centers to cut staff.
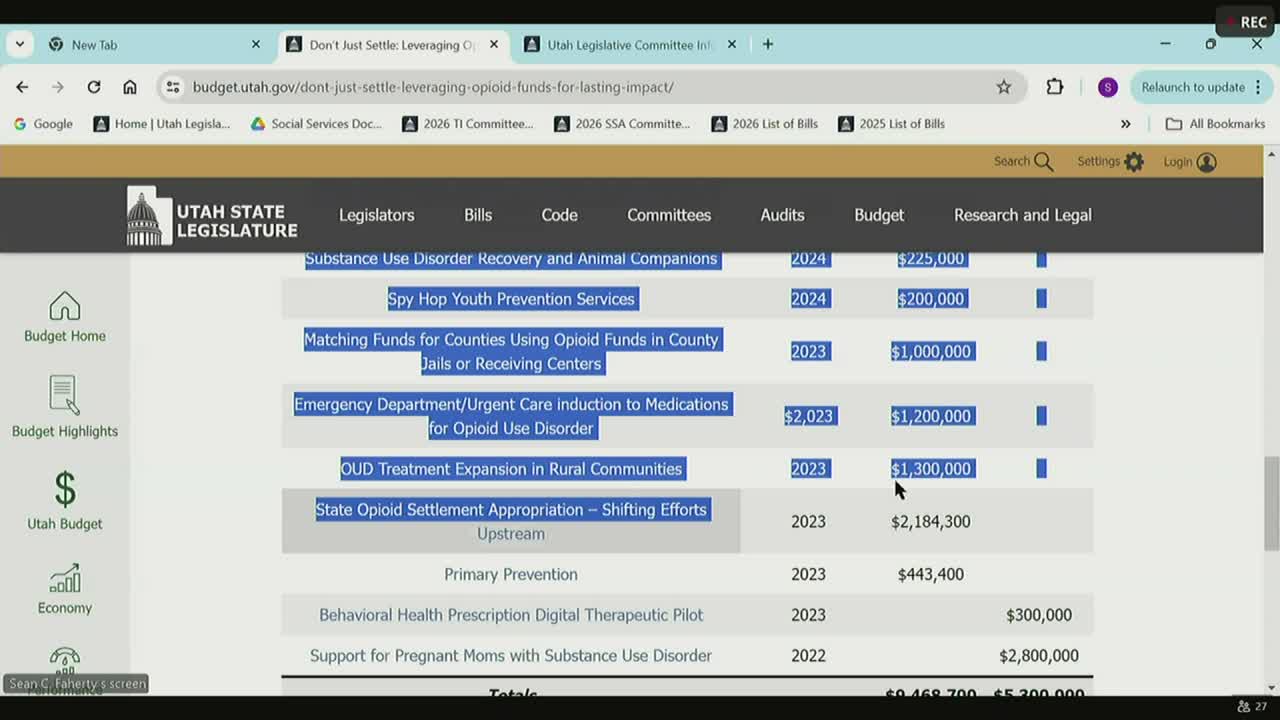
Jail‑based MAT and emergency department initiatives. Randy Huntington (Wasatch Behavioral Health) reported the county jail MAT initiative served roughly 3,500 people statewide across participating counties and focused on initiating and continuing MAT in custody and linking people to community care. Intermountain/CommonSpirit/Moab representatives described an emergency department‑led induction program (the "Compass" program) that provided hundreds of MOUD starts, naloxone co‑prescriptions and peer support services; presenters said the program exceeded grant targets and improved post‑encounter transitions to care.
What lawmakers asked. Committee members sought outcome metrics, sustainability plans and asked how programs would scale if settlement dollars declined. Presenters emphasized the importance of ongoing funding to retain staff and maintain care for rural and uninsured populations.
Next steps. Presenters asked the committee to consider continued or replacement funding strategies as opioid‑settlement grant cycles expire; staff noted a limited pool of remaining settlement dollars in the current cycle.