Get AI Briefings, Transcripts & Alerts on Local & National Government Meetings — Forever.
CMS lays out RY2027 PERM schedule, key state deadlines and responsibilities
Loading...
Summary
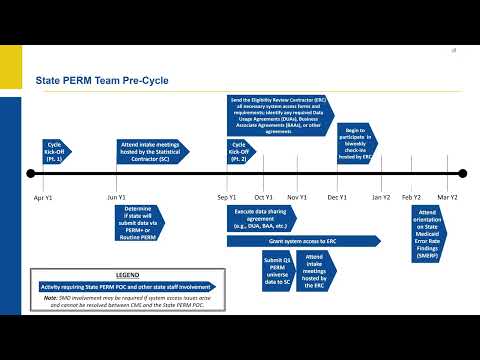
The Centers for Medicare & Medicaid Services (CMS) presented a 36-month RY2027 Payment Error Rate Measurement (PERM) timeline covering precycle, review and closeout phases, contractor roles, data-submission windows, and points requiring state Medicaid director involvement.
The Centers for Medicare & Medicaid Services (CMS) presenter outlined the RY2027 Payment Error Rate Measurement (PERM) cycle and the timeline states must follow to complete eligibility reviews and reporting.
CMS said the PERM cycle spans 36 months and uses a 17–18 state rotation so each state is reviewed once every three years, with a new reporting cycle beginning each spring. The agency described the cycle’s three phases—precycle, review and closeout—and identified milestones and windows for data submissions, sampling, review activity and corrective-action planning.
Why it matters: States’ PERM points of contact and Medicaid directors must meet several hard deadlines to ensure timely reviews and accurate reporting of improper payment rates. CMS warned it may escalate access problems to state Medicaid directors if PERM contractors cannot obtain needed system access.
Key deadlines and responsibilities included: states start the precycle phase in spring of Year 1 with a two-part kickoff (part 1 in April and part 2 in September); states should grant system access to PERM contractors (SC and ERC) as early as September of Year 1 but no later than February of Year 2; states submit universe data to the SC between October of Year 1 and February of Year 2; the SC delivers samples between February and October of Year 2; initial case reviews conclude with a cycle cutoff in April of Year 3; closeout activities and reporting run May–November of Year 3; and state Medicaid directors participate in corrective action plan (CAP) development from December Year 3 through February Year 4.
Contractor roles: The presenter described two contractor types: the PERM statistical contractor (SC), which handles data submission, sampling and initial reporting, and the PERM eligibility review contractor (ERC), which conducts eligibility reviews, manages additional documentation requests (ADRs), processes different resolutions (DRs) and handles appeals. CMS also noted states must execute required data-sharing agreements—such as DUAs or BAAs—during the precycle period and attend intake meetings hosted by the SC and ERC.
Reporting and outputs: CMS said the ERC compiles review results and prepares cycle summary reports (CSRs) including national and state payment error rates; in November of Year 3 state Medicaid directors will see published improper payment rates in the HHS Agency Financial Report (AFR) and will receive the FEFR report as named in the presentation. CMS emphasized that some closeout tasks require only state PERM points of contact, while others require the state Medicaid director’s direct involvement.
State action items and cautions: The presenter urged states to (1) provide timely system access to contractors, (2) execute any necessary DUAs/BAAs promptly, (3) respond to SC and ERC requests for documentation and questions throughout Year 2, and (4) review mid-cycle and final reports when issued. CMS noted that failure to provide timely access or responses could prompt elevation to the state Medicaid director.
The overview closed with an instruction to direct questions to the CMS PERM liaison.