Lifetime Citizen Portal Access — AI Briefings, Alerts & Unlimited Follows
DHSS orientation highlights big Medicaid and child‑care cost changes in FY27 request
Loading...
Summary
DHSS told the Joint Finance Committee the governor's recommended FY27 budget boosts Medicaid funding to address FMAP shifts and projects a $25.27 million child‑care expansion tied to federal rule changes; multiple 1% discretionary requests were not recommended but some larger increases were included.
Department of Health and Social Services officials briefed the Joint Finance Committee on major FY27 budget changes affecting Medicaid, SNAP administration, child care and services for people with developmental disabilities.
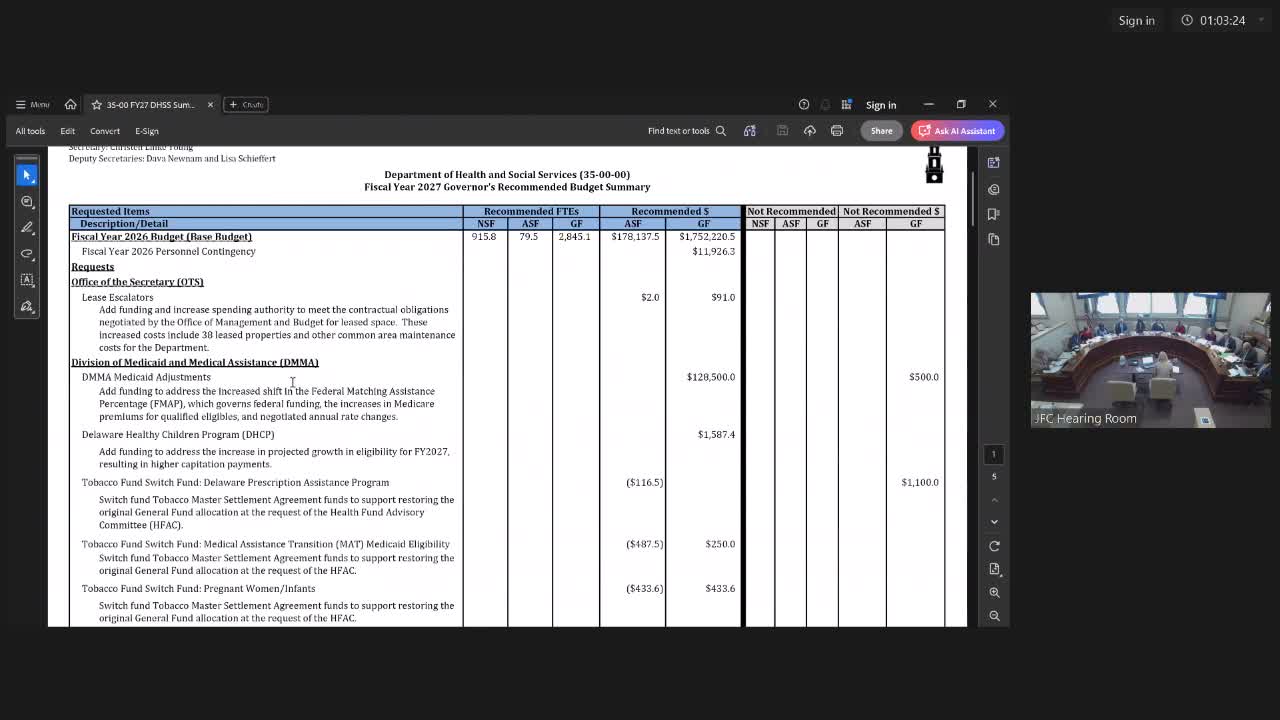
Victoria, DHSS’s presenter, said the governor’s recommended budget includes an approximately $128.5 million recommended adjustment for Medicaid to reflect federal matching rate shifts, increases to capitation payments and negotiated annual rate changes. The department also proposed $25,266,200 to implement new Child Care and Development Fund rules, including a shift to prospective, enrollment‑based payments and an expansion of eligibility to 300% of the federal poverty level.
DHSS outlined a series of fund‑switch proposals tied to the Tobacco Master Settlement Agreement that would reduce ASF authority and restore general‑fund allocations for programs such as the Prescription Assistance Program and services for pregnant women and infants. The department also recommended an ongoing $10.58 million for direct support professional (DSP) rate increases aligned with the McNesby Act; that increase appears in the governor’s recommendation at $10,500,000.
Victoria said DHSS requested $2,000,000 in one‑time funding reserved by OMB for lead remediation and another $1,500,000 for health eligibility and lifeline programming at state service centers. The department included technology upgrades such as a SmartCom cloud migration to support notices and an electronic visit verification maintenance request tied to federally mandated provider systems.
Committee members pressed for more detail on vacancies, rate studies and the SNAP administrative cost increase (a projected $9.23 million state match adjustment), and asked DHSS to provide a ten‑year history of rate changes and a current map of outstanding rate studies before the Monday markup. OMB said it is compiling rate‑study timelines and staffing analyses to assist the committee’s review.
Members flagged several not‑recommended 1% discretionary requests — including Medicaid renewals support and direct funding for certain behavioral‑health provider rate increases — and asked for follow up on implementation logistics and eligibility assumptions for the child‑care changes.
The committee scheduled follow‑up questions to appear in the formal Monday markup packet, including requests for enrollment counts, vacancy lists and rate‑study statuses.